Common symptoms of food allergies and 6 ways to reduce them
![]()
 Food allergy is one of the immune diseases that constitute a serious health problem worldwide. An estimated one-fifth of the population believe they have adverse reactions to food, but the actual prevalence of food allergies varies between 3% and 4% of the world’s population.
Food allergy is one of the immune diseases that constitute a serious health problem worldwide. An estimated one-fifth of the population believe they have adverse reactions to food, but the actual prevalence of food allergies varies between 3% and 4% of the world’s population.
Despite the seriousness of the risks of allergic reactions – which in extreme cases can cause death – there is unfortunately no current treatment for food allergy. The only cure is prevention!
Trying to avoid allergens or, in the event of an allergy, treating the symptoms remains the only option available for the time being.
Fortunately, there are natural ways to reduce food allergy.
These can help stimulate the immune system and improve the intestinal microbiota, helping to reduce the development of food allergies and thus their symptoms.
What is a food allergy?
A food allergy is the immune system’s response to an unpleasant food.
In other words, when the body detects that a particular compound in a food may be dangerous, it triggers an immune system reaction to protect itself by producing histamine.
The body memorizes this substance as dangerous, and when it is consumed again, its defense process is immediately triggered.
Food intolerance vs. food allergy
Diagnosing food allergies can be problematic, as non-allergic food reactions, such as food intolerance, are often confused with food allergy symptoms.
Food allergies and intolerances are often linked, but there is a clear difference between the two conditions.
Intolerance derived from an immunological mechanism is called food allergy, and the non-immunological form is called food intolerance.
A food allergy results from a reaction of the allergen-specific immunoglobulin E antibody in the bloodstream.
Non-IgE-mediated food allergies are also possible.
This occurs when someone is exposed to a food that causes signs and symptoms of allergy, such as allergic contact dermatitis.
A food intolerance is an adverse reaction to food or food components, but which is not due to immunological mechanisms.
For example, a person may have an immunological response to cow’s milk because of the milk protein, or that person may be milk intolerant because of an inability to digest lactose.
The inability to digest lactose leads to excessive fluid production in the gastrointestinal tract, resulting in abdominal pain and diarrhea.
This condition is called lactose intolerance because lactose is not an allergen and the response is not immune. [1]
Food intolerances are non-specific and symptoms often resemble common medically unexplained complaints, such as digestive problems. [2]
Common food allergies
IgE food allergies are the most frequent and most dangerous adverse food reactions.
They cause the immune system to react abnormally when exposed to one or more specific foods.
Immediate IgE-mediated food allergy reactions are caused by an allergen-specific anti-immunoglobulin E antibody in the bloodstream.
When IgE is functioning properly, it identifies triggers that could be harmful to the body, such as parasites, and therefore signals the body to release histamine.
Histamine causes allergy symptoms such as hives, coughing and wheezing.
Sometimes, IgE reacts to normal proteins found in food, and when the protein is absorbed during digestion and enters the bloodstream, the whole body reacts as if the protein were a threat.
This is why food allergy symptoms can be felt in the skin, respiratory, digestive and circulatory systems.
Prevalence of food allergies
According to a comprehensive 2014 review published in Clinical Journals in Allergy and Immunology, the prevalence of food allergy in infants is increasing and can affect up to 15-20% of infants. [3]
And researchers at Mount Sinai School of Medicine suggest that food allergies affect up to 6% of young children and 3-4% of adults [4].
This alarming increase in this rate calls for a public health approach to the prevention and treatment of food allergy, particularly in children.
Researchers suggest that this increase in the prevalence of food allergy may be due to a change in the composition, richness and balance of the microbiota that colonize the human gut in early childhood.
The human microbiome plays an essential role in the development and function of the immune system early in life.
Since IgE-mediated food allergies are associated with immune dysregulation and altered intestinal integrity, there is substantial interest in the potential link between gut microbiota and food allergies. [5].
The 8 most common food allergies
Although any food can provoke a reaction, relatively few foods are responsible for the vast majority of significant food-induced allergic reactions.
Over 90% of food allergies are caused by the following foods:
1. Cow’s milk
 Allergy to cow’s milk proteins affects 2 to 7.5% of children.
Allergy to cow’s milk proteins affects 2 to 7.5% of children.
Persistence into adulthood is rare, as tolerance develops in 51% of cases within 2 years, and in 80% of cases within 3-4 years. [6].
Many milk proteins have been implicated in allergic responses, and most have been shown to contain multiple allergenic epitopes.
IgE-induced reactions to cow’s milk are common in early childhood, and non-IgE-mediated reactions are frequent in adults.
A study published in 2005 in the Journal of the American College of Nutrition suggests that the prevalence of self-diagnosed cow’s milk allergy is 10 times higher than the clinically proven incidence, suggesting that a large population unnecessarily restricts dairy products (for allergic purposes) [7].
2 Eggs
 After cow’s milk, allergy to hen’s eggs is the second most common food allergy in infants and young children.
After cow’s milk, allergy to hen’s eggs is the second most common food allergy in infants and young children.
A recent meta-analysis of the prevalence of food allergy estimated that egg allergy affects between 0.5% and 2.5% of young children.
Egg allergy usually presents in the second half of the first year of life, with a median age of presentation of 10 months.
Most reactions occur during a child’s first known exposure to egg. Eczema is the most common symptom.
Five major allergenic proteins in domestic chicken eggs have been identified, the most dominant being ovalbumin [8].
3. Soy
 Soy allergy affects around 0.4% of children.
Soy allergy affects around 0.4% of children.
According to a 2010 study at John Hopkins University School of Medicine, 50% of children allergic to soy had overcome their allergy by the age of 7. [9].
The prevalence of sensitization after the use of soy-based formulas is around 8.8%.
Soy formula is commonly used for infants allergic to cow’s milk, and research suggests that soy allergy occurs in only a small minority of young children with IgE [10].
4. Wheat
 Gluten-related disorders, including wheat allergy, celiac disease and non-celiac gluten sensitivity, have an estimated worldwide prevalence close to 5%.
Gluten-related disorders, including wheat allergy, celiac disease and non-celiac gluten sensitivity, have an estimated worldwide prevalence close to 5%.
These disorders share similar symptoms, making a clear diagnosis difficult.
A wheat allergy represents a type of adverse immunological reaction to the proteins contained in wheat and related grains.
IgE antibodies are involved in the inflammatory response to several allergenic proteins present in wheat.
Wheat allergy affects the skin, gastrointestinal tract and respiratory tract.
Wheat allergy is more prevalent in children, who generally outgrow the allergy by school age. [11].
5. Peanuts (peanut or cacahuète)
 Peanut allergy tends to appear early in life, and affected individuals generally do not outgrow it.
Peanut allergy tends to appear early in life, and affected individuals generally do not outgrow it.
In highly sensitive individuals, only traces of peanuts can induce an allergic reaction.
Research suggests that early exposure to peanuts may reduce the risk of developing this allergy.
According to a 2010 study, peanut allergy affects around 1% of children and 0.6% of adults in the United States.
Peanuts are inexpensive and are often consumed in unmodified form, as a component in the preparation of many dishes.
This is why they cause the highest number of cases of severe anaphylaxis and death. [12].
6. Walnuts
 The prevalence of nut allergies continues to rise worldwide, affecting around 1% of the world’s population.
The prevalence of nut allergies continues to rise worldwide, affecting around 1% of the world’s population.
These allergies most often begin in childhood, but can occur at any age.
Only around 10% of people outgrow nut allergies.
And frequent lifelong reactions caused by accidental ingestion are a serious problem. [13].
The nuts most frequently responsible for allergic reactions include hazelnuts, walnuts, cashews and almonds.
Those less frequently associated with allergies include pecans, chestnuts, Brazil nuts, pine nuts, macadamia nuts, pistachio, coconut, Nangai nuts and acorns.
A 2015 systematic review found that walnut and cashew allergies were the most common types of nut allergy.
7. Fish
 According to a study published in Clinical Reviews of Allergy and Immunologyadverse reactions to fish are not only caused by the immune system’s reaction, but are often caused by various toxins and parasites.
According to a study published in Clinical Reviews of Allergy and Immunologyadverse reactions to fish are not only caused by the immune system’s reaction, but are often caused by various toxins and parasites.
Allergic reactions to fish can be serious and even life-threatening.
And children generally don’t outgrow this type of food allergy.
A reaction is not limited to ingesting fish, as it can also be caused by handling fish and ingesting cooking fumes.
Prevalence rates of self-reported fish allergy vary from 0.2 to 2.29% in the general population, but can reach up to 8% in fish processing workers. [14].
8. Crustaceans
 Allergic reactions to shellfish, which include crustacean groups (crabs, lobsters, crayfish, shrimp, krill, woodlice and barnacles) and mollusks (squid, octopus and cuttlefish), can cause clinical symptoms ranging from mild urticaria (hives) and oral allergy syndrome to life-threatening anaphylactic reactions.
Allergic reactions to shellfish, which include crustacean groups (crabs, lobsters, crayfish, shrimp, krill, woodlice and barnacles) and mollusks (squid, octopus and cuttlefish), can cause clinical symptoms ranging from mild urticaria (hives) and oral allergy syndrome to life-threatening anaphylactic reactions.
Mollusc allergy is known to be common and persistent in adults, and can cause anaphylaxis.
The prevalence of shellfish allergy is 0.5 to 5%.
Most children allergic to shellfish are also sensitive to house dust mite and cockroach allergens. [15].
A phenomenon known as cross-reactivity can occur when an antibody reacts not only with the original allergen, but also with a similar allergen.
Cross-reactivity occurs when a food allergen shares a structural or sequence similarity with a different food allergen, which can then trigger an adverse reaction similar to that triggered by the original food allergen.
This is common among different shellfish and nuts [16].
Symptoms of allergic reaction
Symptoms of food allergy can range from mild to severe.
In rare cases, they can lead to an anaphylactic reaction, a severe and potentially fatal allergic reaction.
Anaphylaxis can impair breathing, cause a dramatic drop in blood pressure and alter heart rate.
It can be triggered within minutes of eating an allergenic food.
If a food allergy causes anaphylaxis, it can be fatal and must be treated with an injection of epinephrine (a synthetic version of adrenaline).
Symptoms of food allergy can involve the skin, gastrointestinal tract, cardiovascular system and respiratory tract.
Some common symptoms include:
- Vomiting ;
- Stomach cramps;
- Coughing;
- Wheezing;
- Shortness of breath;
- Difficulty swallowing
- Swelling of the tongue ;
- Inability to speak or breathe;
- Weak pulse;
- Dizziness;
- Pale or blue skin.
Most food allergy symptoms occur within two hours of consuming the allergen, and often begin within a few minutes. [17].
Exercise-induced food allergy occurs when ingestion of a food allergen causes a reaction during exercise.
When you exercise, your body temperature rises, and if you consumed an allergen just before exercising, you may develop hives, itchiness or even feel dizzy.
The best way to avoid exercise-induced food allergy is to completely avoid the food allergen for at least 4 to 5 hours before any exercise [18].
Food allergy test
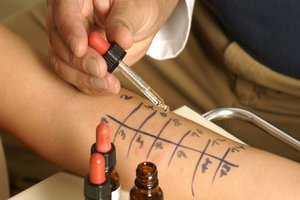 A systematic approach to diagnosis includes careful consultation of the medical history, followed by laboratory tests, elimination diets to confirm the diagnosis.
A systematic approach to diagnosis includes careful consultation of the medical history, followed by laboratory tests, elimination diets to confirm the diagnosis.
It’s important to be assessed and diagnosed by a healthcare professional or allergist.
Self-diagnosis of food allergies can lead to unnecessary dietary restrictions and inadequate nutrition, particularly in children.
Recently, an increasing number of commercial food allergy tests are being marketed to consumers and healthcare professionals.
IgG or food intolerance tests aim to identify food sensitivities, food intolerances or food allergies, but researchers believe that this is an unvalidated form of testing.
The test checks blood levels of immunoglobulin G (IgG) – an antibody created by the body to fight certain allergenic foods.
Blood samples are exposed in vitro to a panel of foods and food components.
The degree of binding of the total IgG antibody to each food is measured to determine which of the foods creates an immune response.
The degree of sensitivity or allergy is then classified on a rating scale.
The problem with this type of food allergy testing is that, unlike IgE antibodies, which are responsible for allergies, IgG antibodies are found in both allergic and non-allergic individuals.
IgG antibodies are the normal antibodies produced by the body to fight infection.
Researchers believe that the presence of food-specific IgG is in fact a marker of exposure and tolerance to food, and not necessarily a sign of allergy.
Therefore, positive test results for food-specific IgG remain possible in normal, healthy adults and children.
For this reason, the likelihood of false diagnoses is too high, and people could be misled by the information provided by such food intolerance tests.
In addition, and because of the potential misuse of this type of test, there is controversy surrounding food sensitivity tests, and many researchers believe that these tests are not appropriate for making a diagnosis of food allergy.
IgG testing can also make parents anxious, especially if the test is intended for their child and the result is positive. [19].
According to a study published in Allergy, Asthma & Clinical Immunologythe greatest risk of this type of testing is that a person with a genuine IgE food allergy, who is at high risk of life-threatening anaphylaxis, may well fail to obtain a result that shows his high levels of IgG specific to his particular allergen.
He may therefore be ill-advised and at risk of reintroducing this potentially fatal allergen into his diet. [20].
Instead of relying on self-diagnosis or unapproved tests, consult an allergist who will begin by conducting a full medical screening.
After a consultation of the medical history, an allergist will usually carry out a combination of tests that will give him enough information to provide a correct diagnosis.
These tests may include a skin test, a blood test, an oral food test and a food elimination diet. [21].
6 ways to reduce food allergy symptoms
There is currently no treatment available to prevent or treat food allergies.
Managing food allergies involves avoiding ingestion of the responsible allergen and knowing what to do in the event of unintentional ingestion.
The following natural treatments for food allergies will help you cope with food allergy symptoms and make them less severe.
1. The GAPS diet
The GAPS diet is a meal plan designed to repair the intestinal lining, stimulate the immune system, stop toxic overload and prevent toxins from entering the bloodstream.
It is commonly used in the treatment of autoimmune diseases.
The diet focuses on eliminating foods that are difficult to digest and damaging to the intestinal flora.
It tends to replace them with nutrient-rich foods to give the intestinal mucosa a chance to heal and seal in its natural balance. [22].
As part of the GAPS diet, you should avoid processed foods, grains, processed sugar, starchy carbohydrates and potatoes, artificial chemicals and preservatives, as well as conventional meat and dairy products.
Instead of eating these inflammatory foods, focus on eating healing foods such as bone broth, non-starchy vegetables, organic wild meats, healthy fats and probiotic-rich foods.
2. Digestive enzymes
Incomplete digestion of food proteins can be linked to food allergies and can cause gastrointestinal symptoms.
Taking digestive enzymes with meals can help the digestive system to completely break down food particles.
It also serves as a vital remedy against food allergies.
3. Probiotics
Probiotic supplements boost immune function and reduce the risk of developing food allergies.
A 2011 study published in Bioscience of Microbiota, Food and Health evaluated 230 infants with suspected cow’s milk allergy.
The infants were randomly divided into groups that received a mixture of four probiotic strains or a placebo for four weeks.
Results showed that probiotics can improve both inflammation and gut immune defense.
Probiotic treatment further stimulated immune system maturation, as infants given probiotics showed increased resistance to respiratory infections and a better vaccine antibody response. [23]
4. MSM (methylsulfonylmethane)
Research suggests that MSM supplements may be effective in reducing allergy symptoms.
MSM is a sulfur-containing organic compound that is used to improve immune function, reduce inflammation and help restore healthy body tissue.
It can be used to relieve digestive problems and skin conditions associated with allergy symptoms. [24].
5. Vitamin B5
Vitamin B5 supports adrenal function and can help control food allergy symptoms.
It is important for maintaining a healthy digestive tract and stimulating immune function. [25].
6. L-glutamine
L-glutamine is the most abundant amino acid in the blood, and can help repair leaky gut and boost immune health.
Research indicates that leaky gut, or intestinal hyperpermeability, is likely to cause a variety of pathologies, including allergies.
Compounds such as L-glutamine have the mechanistic potential to inhibit inflammation and oxidative stress [26].