A reliable source on many subjects.

A reliable source on many subjects.

![]()
 Sleeve gastrectomy, also known as bariatric surgery, is one of the most widely performed surgical techniques, along with bypass, gastric banding and intragastric ballooning.
Sleeve gastrectomy, also known as bariatric surgery, is one of the most widely performed surgical techniques, along with bypass, gastric banding and intragastric ballooning.
With gastric banding, we have already discussed the surgical solutions available to combat obesity (see our article on gastric banding HERE).
With obesity on the increase, and becoming a major national and international health problem, medical research is very active in finding solutions to help sufferers.
Today, sleeve surgery is the most popular anti-obesity procedure, and is often wrongly presented as a miracle operation because it enables rapid weight loss within the first few months.
Our article takes a closer look at this famous operation for you.
Sleeving, like other obesity surgery operations, is intended for people suffering from severe obesity, known as morbid obesity. The BMI must be over 40, or 35 if the person suffers from weight-related disorders (diabetes, sleep apnea, etc.). But that’s not all, and other conditions must be met to qualify for a sleeve.
 Sleeve surgery involves restricting food intake to reduce daily calorie intake.
Sleeve surgery involves restricting food intake to reduce daily calorie intake.
To achieve this, the operation will surgically shrink the size of the stomach, requiring the patient to eat only small quantities of food, more often.
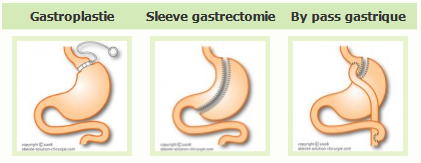
The operation itself will cut the pouch of the stomach so that it forms a kind of sleeve. The remaining tube is stapled along the entire length of the stomach to close it. With the stomach shrunk in this way, it is simply impossible to ingest a lot of food at once.
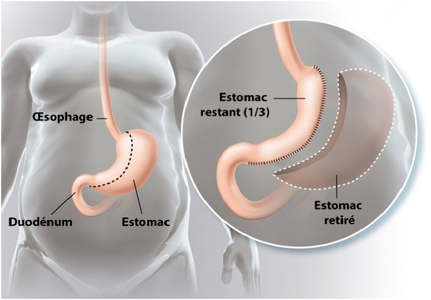
Sleeving is an irreversible operation (unlike gastric banding, for example), as part of the stomach is simply removed.
The operation generally lasts between 1 and 3 hours, and requires a hospital stay of around 5 days.
Here is a brief description of the Sleeve procedure:
As this operation is irreversible, it is essential to be well prepared.
Indeed, undergoing such an operation and losing several dozen kilos in a short space of time has major consequences. Whether in terms of body image, social relationships or changes in eating habits, the change is significant and must be the subject of real reflection and thorough preparation.
Several months before the operation, a number of meetings with different health professionals and members are necessary.
The patient will consult an endocrinologist, a psychiatrist, a dietician, a gastroenterologist, a cardiologist, a pneumologist, a radiologist, an anesthetist and the surgeon in charge of the operation.
Various examinations (blood tests, electrocardiogram, gastroscopy, abdominal and cardiac ultrasound, functional respiratory exploration, X-rays) will enable us to establish :
Hospitalisation for sleeve surgery is scheduled either the day before, for operation the following morning, or the morning, for operation the same day.
In the former case, patients fast from midnight onwards; in the latter, a light breakfast may be taken before 8am.
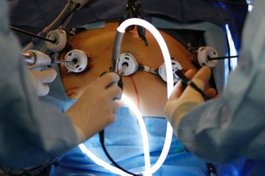
The operation is performed under general anaesthetic by laparoscopy.
After the operation, the patient goes into recovery and remains hospitalized for 5 days.
A small tube (called a Redon) is installed at the end of the operation. It exits through a small opening in the abdominal wall, and is designed to aspirate secretions associated with the operation.
The Redon is removed 2 to 3 days after the operation.
Painkillers are also prescribed, first intravenously, then orally, to alleviate post-operative pain.
Eating is impossible for several days after the operation, and the surgeon may agree to a glass of water the day after the operation.
A physiotherapist is also on hand to help the patient sit up and offer gentle sitting exercises.
After the operation, it is essential to resume eating gradually, so as not to fill the healing stomach.
Here are some general guidelines for post-operative nutrition:
– Week 1: The week begins with exclusively liquid foods (water, tea, broths), then is gradually thickened with thick soups, fluid purées, compotes, yoghurts, fromage frais or even jars of baby food.
– Weeks 2 and 3: Soft-textured foods, neither too dry nor too stringy (e.g. cooked apples, ratatouille, scrambled eggs, etc.).
– Week 4: Return to a normal, controlled diet.
It’s essential to eat slowly, and to stop at the first indicators of satiety.
After the 1st month :
Close follow-up with a dietician, or with your GP, will help avoid vitamin and trace element deficiencies.
But also:
Sleeving leads to major changes.
Autonomy of movement, often impeded in cases of severe obesity, is gradually restored; problems linked to excess weight diminish, and in many cases disappear completely (snoring, sleep apnea, etc.); the sensation of hunger is reduced.
In concrete terms, daily life after sleeve surgery changes radically, particularly with regard to meals.
The sensation of satiety occurs after just a few mouthfuls, and the quantity of food consumed is generally equivalent to 1 pot of yoghurt per meal.
The scales will gradually show significant weight loss, enabling a return to a more active lifestyle and greater self-confidence.
The whole relationship with one’s body, one’s image, but also with others, evolves.
Complications following sleeve surgery are rare, but can be serious. There are 3 main complications:
Opinions on sleeve surgery are divided.
The operation is now widely practiced in France (13,000 people underwent it in 2011), but unfortunately not always according to the right indications.
It is important to be aware of the serious consequences of sleeve surgery, and not to believe that it represents a miracle solution.
Sleeving in no way dispenses with a radical change in eating and exercise habits.
Complications are not inexistent, and the operation is irreversible, which is a real drawback. Another factor not to be overlooked is the high cost of the operation!
Only after careful consideration of your personal situation should you make such a decision.